It’s been a while… life (not just diabetes) has gotten in the way.
Technology has undoubtably changed the way that diabetes is managed. We are lucky to live in the modern world with access to this tech but it isn’t without its faults.
History of Technology
Prior to the 1980s patients could only manage their blood glucose levels using urine, a slow and inaccurate way of measuring such an important thing.
A lot has changed in the past 20 years with the first Continuous Glucose Monitor (CGM) for real-time monitoring being approved for use in 2006.
Fast forward 10 years to 2016 and the first ‘artificial pancreas’ – a hybrid-closed loop system was approved for use by the FDA in America. I will come back to the hybrid-closed loop later.
Recent history shows that it really has been a busy time for research in diabetes management.
Hybrid Closed-Loop System (HCL)
Some people may know them as an ‘artificial pancreas’, although I’m not sure I would deem this an accurate term. It makes it sound like it can mimic the function of a pancreas exactly. Let’s face it, the body is an amazing thing (when it works), I’m not sure how easy it will be to ever mimic its function exactly.
A HCL system is when a CGM and insulin pump are linked. The pump uses the data of blood glucose levels provided by a CGM to automatically adjust how much ‘background’ insulin is given based on an algorithm. Whilst this works away in the background, there is still a requirement to input the carb content of any food/drink consumed and therefore give insulin via the pump.

This system is life-changing for many. It reduces the requirement for multiple injections a day, can reduce the mental burden and can improve blood glucose management. In 2024 the use of HCL was rolled out across the NHS and luckily children are eligible; T was started on this system the second day that he was under Birmingham’s care.
Continuous Glucose Monitors (CGMs)
There are various CGMs available on the market, each connecting to different insulin pumps (to create a hybrid closed-loop) but T uses a Dexcom G6. If you are someone living with or supporting someone with T1D then you might be aware that this is due to be phased out later in the year….
Why does he use a G6?
Essentially, he was started on it when his care moved back to Birmingham but primarily, it can be used alongside the Omnipod 5 (his insulin pump). Changed every 10 days, it has a ‘warm-up’ time of 2 hours, meaning that once placed, it takes 2 hours to provide any readings. After being used to having new readings every 5 minutes, 2 hours without information (unless doing a finger prick test) feels like a lifetime, a downside of technology.
Whilst the G6 is reported to be an accurate sensor, we have come to realise that this isn’t always the case… Even as I sit here writing this, the sensor is reading differently to what his finger prick test is telling us. Sensors can mis-read, and when you are making decisions about whether to give more insulin, it can be quite a dangerous thing.
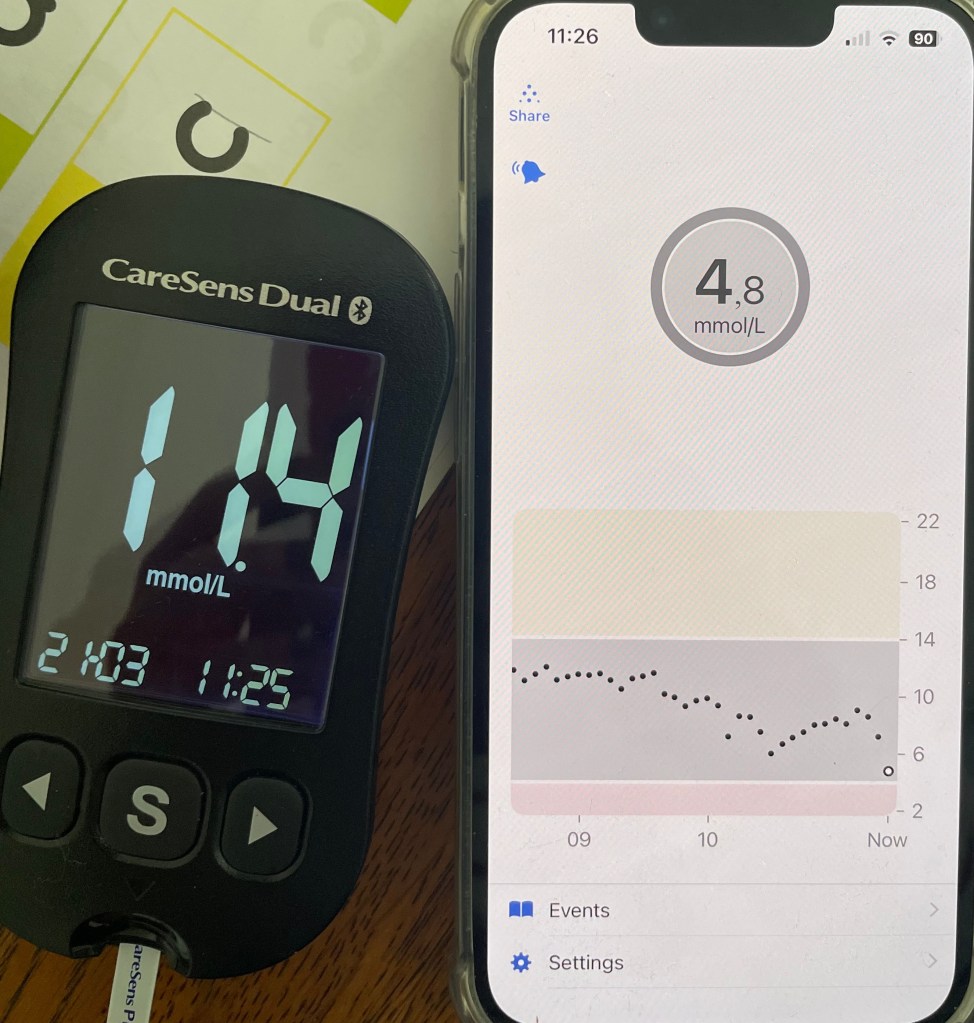
Or, when the sensor casually decides to stop working at a really inopportune moment…
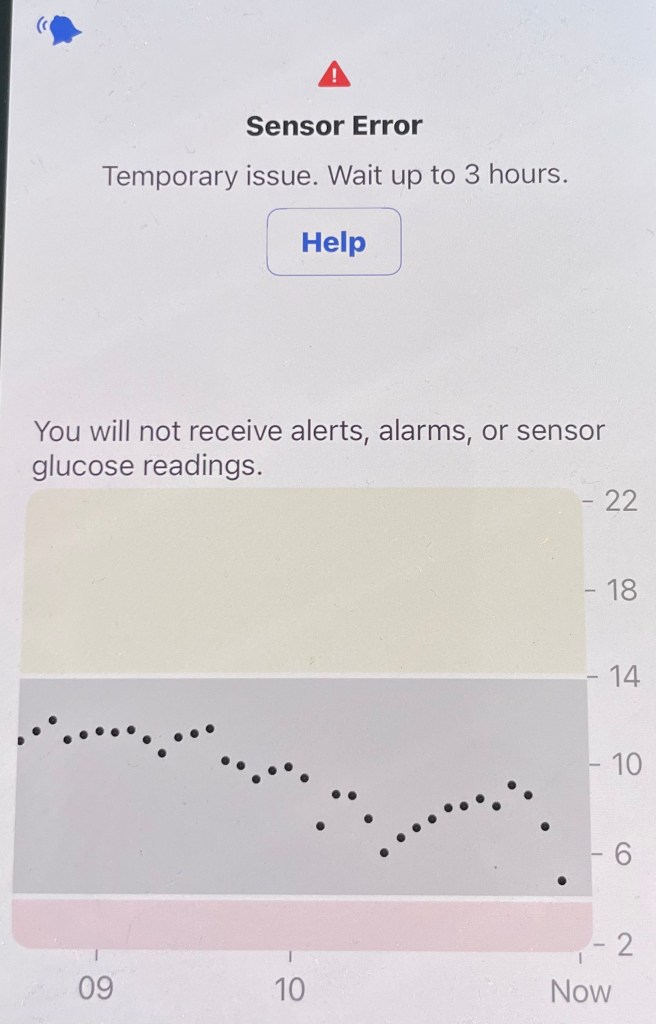
Insulin Pump
The final component on the HCL is the insulin pump. T uses an Omnipod 5, a ‘pod’ style pump. Changed every 72 hours, stuck directly on the skin with no tubes and waterproof for up to 60 mins, pretty great overall. T might not agree as he really isn’t a fan with the ‘click’ as the cannula is inserted, fair enough. However, when he is older, I’m sure he will appreciate the positive aspects more.

Overall, we have had a good experience but they do like to stop working at inopportune times, like down the beach when you forgot to bring the spray to remove the sticky, or when you have arrived at a Eurocamp late at night. Fun times! We even had to change his pump at 0230 when Theo is asleep and levels just keep rising no matter how much insulin you think you are putting in. I think that every time we have been away a pump has needed to be changed early. It almost puts us off going away… However, we are learning the importance of being prepared for everything and having lots of spare things on us!
I am proud of the way that T isn’t afraid to show others his pump and CGM, they are on show most of the time and if people ask about them, he is always happy to speak about what they do. Yes, it’s an invisible illness but I think that it is important to be open about it, not only because others are more likely to look out for him, but it is also important to raise awareness of this life changing illness.
Until next time.
Lx


Leave a comment